Toronto’s 30 Best Doctors
The hospitals, clinics and specialists providing first-rate care

This city is the hub of medical research in Canada, with dozens of state-of-the-art facilities and new labs opening all the time. And Torontonians are the lucky beneficiaries, with access to fantastically talented doctors—they’re the stars of the medical world and the people who may well save your life.
Below, we profile these stars—the city’s top physicians. To assemble the list, we spoke to prominent figures in the city’s medical community and polled nearly 1,000 Toronto doctors, asking them to nominate the best practitioners in prominent specialties—everything from cancer care to urology. We asked respondents to take into account a nominee’s skills, reputation and contributions to a medical field. Here are the doctors other doctors would trust with their lives.
Doctor headshots courtesy of their respective institutions
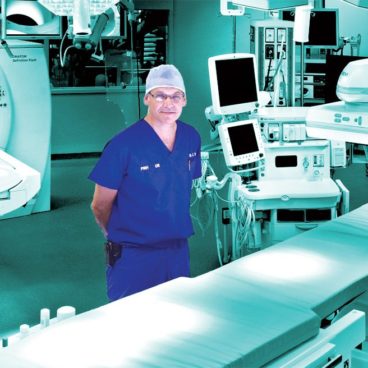
surgical oncology
Chief of surgical oncology,
Princess Margaret Cancer Centre
The slick new OR that Jonathan Irish opened at Toronto General features one of the most advanced surgery technologies out there: a mounted moveable CT scanner that slides across the entire length of a patient’s body, capturing real-time 3-D images that help surgeons like Irish manoeuvre slender and amazingly dextrous robotic arms fluidly inside the body. Irish works on patients with cancers that are hard to get at or too small to see, or that border sensitive tissues. He’s had huge success removing miniscule tumours—visible only via the CT images—and he’s operated on advanced cancers of the head and neck, which are now easier to access through the nostril or skull base. Irish and his colleagues have performed over 50 of these surgeries since the OR launched last year. For patients lying amid this pile of impressive hardware, it all amounts to early intervention, less cutting and pain, quicker recovery, and a good chance you won’t have to come back.
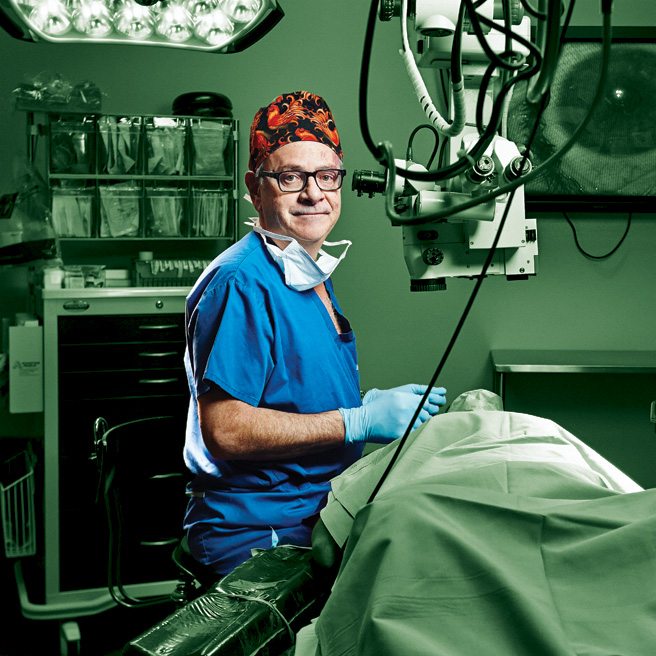
eye surgery
Research director of the Cornea,
Service, UHN
Limbal stem cell disease delivers a swift one-two punch: blindness and severe, stabbing eye pain. In 2010, when Allan Slomovic confirmed that a young Queen’s student named Taylor Binns had the rare disease, Binns had been suffering for more than two years. Slomovic decided a stem cell transplant was his only hope. The procedure involved harvesting stem cells from Binns’s sister’s eye, then attaching them to Binns’s damaged cornea with a bit of tissue glue and tiny stitches. The stem cells worked their regenerative magic, replacing Binns’s diseased cells. A month later, he was pain-free and able to drive a car. It was the first surgery of its kind performed in Canada. Since then, Slomovic has also developed the hospital’s new cornea replacement program and is working to bring over a pioneering prosthetic therapeutic ocular lens from Boston, all part of his grand plan to make UHN the country’s go-to ocular regenerative program.

Brain Surgery
Interim head of neurosurgery,
Sunnybrook
He’s young by brain surgeon standards and has made a name in the risky field of tumour surgery, where many patients have fewer than 15 months to live. If Mainprize’s clinical trials go well, Sunnybrook could soon be offering a groundbreaking treatment for brain tumours buried deep in the skull. He uses a Jetsons-esque helmet to zap tumours with powerful ultrasound waves without a single incision and without overheating the skull. To keep the skull temperature down, over 1,000 probes send ultrasound waves via separate trajectories, and once they’ve penetrated the bone they converge into one searing point that chars the tumour. The helmet can also be used to disrupt the protective blood-brain barrier, allowing chemotherapy to travel to the brain’s innermost reaches. It all sounds a bit kooky, Mainprize will admit, but he sees this as a huge advancement for treating not only brain cancer, but also potentially depression, schizophrenia and Alzheimer’s—any neurological disease for which powerful medications could ride the ultrasound waves directly into the brain.

Pediatrics
Pediatrician-in-chief and director of the Maternal Infant Care Research Centre,
Mount Sinai
Thirty years ago, parents with very sick or pre-term infants were shut out of the neonatal intensive care unit, their noses literally pressed to the glass, watching as their babies were swaddled, soothed and attended to by hospital staff. Lee, an accomplished neonatologist wooed to Sinai from Alberta, not only welcomed parents into the NICU, he tasked them with daily charting and monitoring, and actively consulted them in all decision-making. His Family Integrated Care Program, launched in 2011, was the first in North America to incorporate this level of parental care. Today, as Lee makes his NICU rounds, monitoring preemies’ ventilation and prescribing life-saving treatments, he is aided by the keenly observed insights only a parent could glean. Trial studies showed that the parent-cared babies at Lee’s clinic gained more weight and suffered fewer infections compared with babies only under nursing care. The study has expanded to 20 other hospitals in Canada, and if results are favourable, we may be looking at a new standard of care, not just in neonatal ICUs, but in other areas of pediatrics as well.

Heart Surgery
Director of the Heart Transplant Program,
Peter Munk Cardiac Centre, UHN
At one of the province’s most advanced heart clinics, Ross sees the worst-off cardiac patients whose hearts won’t let them walk stairs or get dressed without gasping for air. After she exhausts all treatment options (medications, bypass surgery, angioplasty), Ross shepherds patients through the long transplant process. One young mother came to her a few years ago with a rare and severe heart disorder. She was too sick for a mechanical heart (often used as a temporary bridge to transplantation), plus she was tiny, so finding a small heart was an additional challenge. For several months Ross kept the patient’s heart pumping and her spirits high, until a donor finally came through. When Ross isn’t saving the brokenhearted, she fronts an R&B band, appropriately called the Marginal Donors.

Head of cardiovascular surgery,
UHN
This veteran surgeon and once-mentor to Dr. Oz has performed 14,000 open-heart surgeries and invented some 20 surgical techniques, largely in the field of heart-valve repair. One procedure, aptly called the David Operation, he came up with in the OR when he realized the patient’s aortic valve, when cleared of scar tissue, didn’t need replacing but some light support with a plastic tube. Today, 20 years after that pioneering surgery, it’s standard treatment all over the world. David’s colleagues and students speak of the “Tirone factor” when describing his surgical creativity. He’s also known for beyond-the-call bedside care, staying late into the night to ensure his patient is in the clear. Though retirement is a niggle in the back of his mind, David is still a fixture in the OR and continues to tinker in the lab with new therapies in his exhaustive effort to improve heart-valve treatments.

Director,
Sussman Allergy and Immunology Clinic
In the 1980s, Sussman was one of the guys who discovered latex allergies, among the most significant allergy findings in decades. Reactions were mistaken for epidemics in hospitals until Sussman’s research pinpointed the source of the allergy (a protein in the gloves). He worked with the latex industry and government to remove the offending ingredient, and today latex allergies cause barely a whimper. Lately, Sussman has been focused on peanuts and ways to desensitize the severely allergic. His clinical trials had anaphylactic patients, both kids and adults, eating increasing doses of peanut flour, then eventually whole peanuts. Today, he treats a handful of patients this way, offering some assurance that they won’t die if they mistakenly eat a peanut crumb on a restaurant salad. His clinic treats thousands of patients a year for everything from food allergies (most commonly milk, eggs, peanuts and seafood) to chronic hives, and pollen and dust mite allergies.

Staff physician, general internal medicine and clinical pharmacology,
Sunnybrook
A decade ago, when scores of people started showing up in Toronto emergency rooms with dangerously high potassium levels in their blood, which can lead to serious heart problems, David Juurlink discovered many of them had been taking a popular heart drug in combination with a certain blood pressure medication. He sounded the first alarm about the risks of this interaction, and doctors eased up on prescriptions of the heart drug. It’s these sorts of drug interactions and side effects that Juurlink researches, painstakingly teasing patterns from reams of medical records. In addition to solving epidemiological riddles, he also routinely gets called into Sunnybrook’s emergency room or intensive care unit to crack individual patient mysteries, Dr. House–style, like when a middle-aged schizophrenic man with a high fever recently fell into a coma. His doctors tried out treatments for all the plausible causes—everything from heat stroke to any number of infections—before Juurlink landed on the true source: a rare, potentially fatal syndrome triggered by the patient’s antipsychotic medications. Following treatment, the patient was out of intensive care within a week.

Physician, critical care and emergency medicine,
St. Michael’s
Gray’s clinical expertise in both emergency and intensive care is a rare asset in medicine and became crucial when a young patient recently arrived at the St. Michael’s Hospital emergency room with a gunshot wound to the abdomen, the bullet settling in his chest. It was a dire scene the whole way through, and after keeping him alive in the ER, she transferred into the ICU, where she could seamlessly shepherd him through surgery and the dicey recovery period. Gray also plays a major role in the hospital’s ability to respond to crises. After she contracted SARS while on the job in 2003, she began to think about system-wide gaps and unpreparedness. (A decade ago, most hospitals didn’t have pandemic strategies.) She studied disaster planning at Yale and recently wrote the general disaster plan for St. Mike’s, which was tested during the G20 summit, ensuring simple but vital logistical improvements like extra beds and staff on standby.

Director of the non-melanoma skin cancer clinic,
Women’s College
Canadians are more likely to get non-melanoma skin cancer than all other cancers combined. Though it rarely kills people, growth can be fierce and highly disfiguring, and it’s these more aggressive tumours that Nowell Solish deals with on a daily basis. The clinic, which Solish was instrumental in launching in 1993, has become one of the busiest places in the country to treat facial tumours. The process is more difficult because of all the creases and crannies where cancer cells can hide, and because of cosmetic considerations. Solish is a master of Mohs surgery, a cautious approach of cutting out a tumour little by little to preserve as much normal tissue as possible, particularly important in facial surgeries. Patients need only a local anesthetic and a good book. After each surgical removal, they stick around while the lab processes the tissues. If Solish can see unaffected skin on the edges of the tumour, he knows he got it all and the patient is done. If not, it’s back under the scalpel as many times as needed. (Typically it takes Solish three rounds to get it all.) And with a cure rate of 98 per cent, it’s not the worst way to spend a day.

Endocrinologist and director of the
Sick Kids Team Obesity Management Program (STOMP)
Jill Hamilton’s program treats severely obese kids and teens who have added complications like Type 2 diabetes or a brain tumour that is causing rapid weight gain. STOMP is the only pediatric program in Canada to perform bariatric surgery on adolescents—still an uncomfortable idea for many doctors. Of the 150 patients who’ve come through the program since 2010, 20 have had the surgery. One of the first was Nicholas Menecola, a Mississauga teen who maxed out at 340 pounds by the age of 16 and whose chronic leg pain kept him largely immobile. STOMP’s assessment team, led by Hamilton and made up of dietitians and psychologists, deemed Menecola a good candidate based on his circumstances and his aptitude for a total lifestyle overhaul. Three months after surgery, Menecola had lost 80 pounds. After two years, he weighed 189 pounds and was running and cycling daily. Because the surgery is relatively new to this age group, Hamilton has been studying the outcomes, hoping to increase our understanding of the rise of severe obesity.

Head of gastroenterology,
Mount Sinai
The pre-eminent gastro doctor has treated thousands of patients over his 20-year career, and he increasingly sees young people suffering from gut-wrenching bowel conditions like Crohn’s and colitis. And he finds it particularly heartbreaking when women have to battle the decision of whether they can or should have children considering their chronic, often debilitating pain. When an 18-year-old nursing student came to Steinhart with a severe case of Crohn’s, she was malnourished, miserable from the pain and about to drop out of school. Steinhart put the young woman on an IV of Remicade and had one of the centre’s dietitians counsel her on a specialized diet. Food and nutrition play hugely into Steinhart’s treatments (he published a recipe book for Crohn’s and colitis sufferers in 2008). Because she was so sick, he treated her with an anti-inflammatory drug not yet on the market, as well as a specific pair of antibiotics that, in combination, his clinical trials had found to help certain cases. Within two days, the young woman was eating normally and back at school. Last Steinhart heard, she’d finished school, married and had two kids.

Specialist in transplant and surgical oncology,
Toronto General
McGilvray recently opened up a 27-year-old patient to find that his cancer had burned through a portion of his colon and invaded his pancreas as well as the blood vessels supplying his intestines. Twenty years ago this patient would have died; there was no safe surgical solution to get at cancer in the vasculature. Over his young career, McGilvray has honed a unique approach to treat these complex cases, employing the preservation techniques that are used for organ transplants. After removing most of the patient’s abdominal contents, literally piling them on a bench in the OR, McGilvray flushed the organs and intestines with cold preservation fluid, which puts tissues in a latent state long enough to buy time, in this case to carve out the tumours and rebuild the damaged vein using one taken from the patient’s leg (which is a whole other story). Once all the parts were re-implanted and blood began flowing, everything “pinked up,” as they say in the OR, and two weeks later the young patient was home, going over admissions applications—for medical school, no less.

Otolaryngologist-in-chief,
Princess Margaret Cancer Centre and UHN
Microvascular reconstruction is an extremely delicate surgery that uses skin, muscle and bone tissue from the body to rebuild parts of the face, lost usually to cancer. Ralph Gilbert is a trailblazer in the field. Simply removing bone tissue from a shoulder blade, for example, requires detaching muscles and preserving the tiny blood vessels that feed it. To transplant the grafted tissue, Gilbert must reconnect all the miniscule arteries and veins using sutures finer than human hair. He has performed about 70 of these scapula-tissue transplants for upper jaw reconstruction using his own technique, which surgeons worldwide have since adopted. At Princess Margaret, the busiest hospital in the world for this type of surgery, Gilbert has spent his career refining this painstaking, microscopic procedure so that patients walk away not only cancer-free, but also able to speak, chew and swallow.

Director of infection control,
Mount Sinai
McGeer has dealt with SARS, C. difficile and other terrifying superbugs impervious to antibiotics. But what she spends most of her time researching, giving talks and media interviews about, and chairing committees on, is the seasonal flu. She delivers this powerful nugget to whoever will listen: get the flu shot, because you are more likely to die from influenza than any other infectious disease out there—even if you’re young and healthy. Thanks to her exhaustive bullhorning and research on the burdens of influenza among hospital staff, Toronto hospitals are now better at testing sick patients for influenza, which can quietly exacerbate other illnesses and whose symptoms are easily hidden or overshadowed. Not only do patients receive better treatment more quickly, but health care workers know whether to don gloves and face shields. For McGeer, it’s the tracking data that can show just how pervasive and dangerous the flu can be.

Director of the Musculoskeletal and Multisystem Rehab Program,
Toronto Rehab Institute, UHN
Beyond the usual team of physiotherapists and nurses, John Flannery has expanded UHN’s rehab centre to collaborate with occupational therapists, pharmacists, social workers, dietitians and surgeons to be able to repair pretty much any body function imaginable. This stacked approach was put to the test last year, when a 19-year-old patient named Tom Fahlman landed at Flannery’s centre from Regina. He’d had a rare form of sarcoma and, because he was bedridden for nine months, his joints were seized. On top of that, Fahlman’s leg muscles had contracted so much that his toes pulled downward in a permanent ballerina point. Flannery rarely sees someone so young so immobilized; most of his patients are older, recovering from surgeries and discharged within a month. After an oncologist discovered that Fahlman was in remission, Flannery orchestrated a game plan that would resurrect the poor guy: a pharmacist okayed an off-label medication that Flannery used to partially paralyze his calves, so that an orthopaedic surgeon could lengthen and stretch the muscles. Over the course of a year, an army of physiotherapists and nurses got him walking again.

Head of fetal medicine,
Mount Sinai
As surgeries go, fetal operations are some of the toughest, but many of Ryan’s tiny patients suffer from conditions that would be fatal after birth. In 2009, he was part of the team that performed Canada’s first in-utero heart surgery. Guided by ultrasound and using a fine needle, a balloon catheter was threaded into the baby’s heart and inflated to open a restricted valve. Constantly evolving technologies have made fetal heart procedures possible, and surgeons like Ryan are always testing new techniques. After completing animal trials, Ryan, in a world first, successfully inserted a coronary artery stent to create a channel in a blocked membrane between the upper chambers of a fetus’s heart. Not long ago, every baby born with this condition died; today, 50 to 75 per cent of them have better than a fighting chance.

Director of the Marvelle Koffler Breast Centre,
Mount Sinai
She’s a world leader in breast cancer research and one of the reasons Sinai’s Marvelle Koffler Breast Centre exists. When the dedicated breast clinic opened in 1995, it was the country’s first, offering everything from diagnosis to treatment to emotional support. Goodwin works on high-risk and resistant cancers, and has treated a particularly challenging subset of breast cancer patients: young pregnant women. Outside the clinic, Goodwin’s research focuses on risk factors. Her pioneering studies show that women with high insulin levels in their blood (often heavy or obese patients) have worse cancer outcomes, because insulin has a way of switching on breast cancer cells. Her findings have since led to a multinational study of more than 3,500 women to see if taking a common diabetes drug to lower insulin levels will improve survival odds. Thanks to Goodwin’s work, researchers are now studying the effect of insulin on prostate, brain and other cancers, which could lead to remarkably simple, yet important, treatment advances.

Director of renal transplants,
St. Michael’s
Say you want to donate a kidney, but the recipient’s blood type is A, and yours is B. It’s now a viable procedure at St. Michael’s thanks to Zaltzman and his team, who are using an innovative device that allows transplants among incompatible blood types. In this case, the recipient’s blood plasma would be pumped through the device and cleansed of B-antibodies, which would have attacked and ultimately rejected your kidney. This filtration happens a few times before and sometimes after surgery. The laundered blood tricks the body long enough to accept the foreign organ with a little help from immunosuppressive drugs. St. Michael’s—where more than one third of live donors have mismatched blood types—is so far the only hospital in Canada offering this new route out of donor-waiting-list hell.

Director of the Morton and Gloria Shulman Movement Disorders Clinic,
Toronto Western
No Canadian has studied Parkinson’s disease quite like Lang, and it’s impossible to overstate his influence in the field of movement disorders. He built and staffed the clinic at Toronto Western from scratch, starting in the mid-’80s as its sole neurologist. It’s now world renowned and staffed with a team of nine specialized neurologists (hand-picked by Lang) who handle 10,000 patient visits a year from across the globe. Lang’s clinic was the first in North America to treat advanced Parkinson’s with deep brain stimulation using stereotactic neurosurgery, a ’60s-era practice Lang helped refine. Electrodes deliver a high-frequency current to parts of the brain to help tame the tremors and rigidity of Parkinson’s—so drastically for some patients that they could move freely for the first time in years without each step being hijacked by violent jerking.

Site chief of gynecology, Women’s College;
head of gynecology, Mount Sinai;
head of pediatric gynecology, Sick Kids
Allen jokes that she never wears heels to work because of all the running around she might do in a day: performing high-risk gynecological surgeries at Mount Sinai, doing quick outpatient procedures at Women’s College Hospital or treating young girls at Sick Kids who are plagued with everything from ovarian cancers to torsion (a rare “twisting” of the ovary). She most commonly treats girls with heavy or painful periods, which could be a symptom of conditions such as endometriosis. Allen has the kind of deft and delicate bedside manner that’s key when talking to a shy 12-year-old about painful bleeding or vaginal discomfort. Sometimes, she simply has to reassure girls that they’re normal.

Head of orthopaedic surgery,
Mount Sinai
Backstein has been called the Mike Holmes of medicine, because his speciality is fixing knee surgeries gone bad. It’s the toughest kind of orthopaedic surgery, because there’s often significant loss of bone and soft tissue, and more scar tissue to circumvent, while skin and muscles have to be moved around to patch infected areas. He performs a few of these surgeries a week at Sinai, which has become renowned for such complex redos, as well as for having among the shortest knee surgery wait times in the province (70 days). This has a lot to do with Backstein’s constant system tweaks: better-timed pain medication and physiotherapy, and less time on the operating table. Sinai surgeons currently perform more than 600 hip and knee replacements a year. The need for his services will only increase as more of us get older and creakier.

Director of the Centre for Fertility and Reproductive Health,
Mount Sinai
Unlucky couples of a certain demographic will likely recognize the name Greenblatt, a sought-after fertility doctor who’s known for compassion and cutting-edge care. Of the thousands of patients who come through her clinic every year, more than half get pregnant. She sees about 50 new patients a week and, increasingly, cancer patients who want to freeze their eggs, embryos or sperm before undergoing potentially sterilizing chemo, radiation or surgery. Under Greenblatt, Sinai’s fertility centre was one of the first to offer these urgent oncofertility services, and it remains the busiest clinic of its kind in the province. In the lab, she and her colleagues are working on methods to pinpoint the window of time a uterus is most receptive to an embryo—a potentially groundbreaking boost to IVF success rates.

Director of the Wasser Pain Management Centre,
Mount Sinai
When Gordon started Sinai’s pioneering pain clinic in 1999, many doctors still didn’t believe in the existence of fibromyalgia, a syndrome characterized by widespread pain and fatigue, easily dismissed, like many chronic pain conditions, as psychosomatic. Gordon’s clinic is like a warm embrace for people who’ve lived for years with every kind of pain you can imagine: headaches, irritable bowel syndrome, and genital, joint, back and muscle pain. Gordon uses a hospital-wide team of varied specialists offering not only conventional physical treatments (massage, physiotherapy, chiropractic and acupuncture) but also psychiatry and cognitive behavioural therapy to get at pain from all angles. It’s not an approach a recent patient expected when she came to Gordon with debilitating pain. They spent an hour talking about her divorce, depression and alcoholism, which went on to shape the treatment plan: a mix of emotional and physical approaches that work to tackle the acute pain while also arming the patient with long-term coping strategies.

Staff physician, general internal medicine,
Sunnybrook
In 1997, Redelmeier was the first to correlate cellphone use and car accidents using real-world data, and his research went on to inform regulations around the world. (The idea for the study struck while he was on the phone with a patient who crashed his car during the conversation.) His work inspired a slew of studies on driving culture, showing that changing lanes increases your chances of a crash threefold, accidents are more frequent on election days, and getting a traffic ticket decreases your odds of dying in car crash in the following few months by 30 per cent. His knack for drawing conclusions from seemingly random phenomena proves useful for his day-to-day clinical work at Sunnybrook. As an internist, Redelmeier treats people with multiple life-threatening illnesses, for example, a 75-year-old going in for hip-replacement surgery who also has diabetes, hypertension, osteoporosis, a history of cancer and strokes, and chronic kidney disease. It’s Redelmeier’s job to deal with everything but the hip problem. Before surgery, he must determine which of the patient’s dozen medications must be stopped and in what sequence, and which are absolutely essential. He also counsels the family on possible post-op problems, basically attending to all the extra details so the surgeons don’t have to. “I don’t have anything to do with sutures and scalpels,” he says, “but everything else is mine.”

Director of the Ross Tilley Burn Centre,
Sunnybrook
When a young burn victim recently landed in Jeschke’s care, the patient had been languishing in a hospital bed for two years after barely surviving a house fire. Much of his body was still an open, oozing wound. He couldn’t speak or move, and was maxed out on painkillers and antibiotics. Considering the extent of the infection and the absence of even a patch of skin to graft, most surgeons would have turned him away. But Jeschke, in a worldwide first, took a stab at stem cell treatment. He concocted a serum of potent stem cells from donor amniotic fluid, which he applied underneath one of the wounds. When he uncovered the area a week later, the infection had improved enough to allow new skin growth. Within three months, the patient was discharged. Though it was an extremely rare case, Jeschke became thoroughly convinced of the power of stem cells, which he and his team are now using to develop a 3-D skin printer, quite possibly the next revolution in burn treatment.

Radiation oncologist, Odette Cancer Centre,
Sunnybrook
The odds of beating breast cancer these days are so good that some research has veered in the luxurious direction of making treatment more convenient and efficient. Today, because of Pignol’s work on portable radiation, a patient with early-stage breast cancer can walk into Sunnybrook at noon and be done treatment by 1, never having to return. Instead, about 80 tiny radioactive “seeds” are implanted into the tumour. Pignol was the first to apply this highly targeted treatment—already used for certain kinds of prostate cancer—to breast tumours. He’s now testing other treatments that deploy nanoparticles, which are so miniscule they exist somewhere between a solid and a liquid. Similar to the seeds, these gold nanobombs, as they’re called, are inserted into the breast to slowly release radiation, and they can actually follow the natural migration of cancer cells. They eventually dissolve, leaving patients with no trace of the treatment—or the cancer.

Surgeon, oncology and urology,
Princess Margaret Cancer Centre
Finelli specializes in what’s been called minimally invasive prostate surgery. Rather than perform the standard seven-centimetre cut across the abdomen, Finelli, with the help of a robot named da Vinci, can get at the prostate via a few small incisions and remove it through the belly button. He launched the hospital’s urology laparoscopic program nine years ago and proved that such techniques result in less pain and blood loss, and, perhaps most important to patients, a quicker return to regular potency. Finelli performs two robotic prostatectomies a week, and today almost 40 per cent of the hospital’s prostatectomies are done this way, compared with four per cent when Finelli started. The deft touch of a robot has been even more beneficial for surgeries to remove small kidney tumours, which, if done the extremely painful old-fashioned way, require a 10-centimetre incision and, in some cases, a few broken ribs.

Surgeon,
Sick Kids
Langer’s area of interest is surgery on newborns with birth defects, but he does it all: removes kidneys, performs the odd circumcision and treats cancers as well as the gamut of pediatric surgical conditions. And once every few years he gets patients like the Mufuka brothers, Tinashe and Tinotenda, conjoined infant twins from Zimbabwe who captured international media attention when they were flown to Toronto by a medical charity in 2004. They arrived malnourished, attached at the abdomen and liver. Langer had participated in only three twin-separation surgeries throughout his career; they’re extremely rare, highly complex and can often be unsuccessful depending on where the kids are joined. The five-hour surgery went about as smoothly as they go, and after a few months in recovery, the boys, now 10, returned home. Though it was an exceptional kind of surgery, if Langer can expertly deal with conjoined twins, your kid’s appendectomy should be a breeze.

Director of geriatrics,
Mount Sinai and UHN
Sinha is exactly the sort of doctor you want taking care of your aging mother. He spends nearly an hour with every patient on each visit (two hours with new referrals). He makes house calls, about 10 a month, with an old-fashioned medical bag, rooting through patients’ fridges to make sure there’s food, sometimes getting lost in their life stories. Since being recruited from Johns Hopkins three years ago, Sinha has pushed geriatric care to new heights at Sinai by instituting a hospital-wide strategy for elder acute care and ensuring all frontline hospital staff are trained in senior care. He has introduced simple changes, like keeping people mobile, making them get out of bed for meals, and paying more attention to medication combinations and dosages. Under Sinha, the length of hospital stays for the elderly has dropped by 17 per cent, and there have been fewer falls. He was recently selected by the province to lead a seniors strategy on transportation, housing services, job opportunities and elder abuse, so that, as he says, everyone’s golden years are golden.


































Why no pulmonologist? What about lung health?
Can’t believe you have a stereotypical roboquack performing a few too many (ignoring new PSA testing guidelines) prostatectomies at the top of your list. The hair gel should have tipped you off that he is cutting for his own ego instead of the patient.
Benja75, that is a really disrespectful comment to post on the internet. You should be ashamed of yourself. If you are such a critic, why don’t you undergo years of intense medical training and see what contributions you can make to the field of medicine. Congratulations to all of the fine physicians and surgeons whose have been recognized by Toronto life for their dedication to medicine.
I have been a patient of the person in question for over seven years on. He does not ignore PSA guidelines, I have been carefully monitored with biopsies only as appropriate from PSA results. He does not believe in unnecessary invasive procedures. As a result I have been spared the ongoing problems of two of my cousins of approximately the same age and genetic disposition.
Radiation oncology =/= Radiology….
a immediate family member saw Gordon and his team, they never provided any alternate treatment options not other feedback except to get him on methadone and then send through the hoops. It was so bad he luckily avoided a absolute nervous breakdown and had to shop for new docs due to his chronic pain (due to spinal deformation) and basically I can not add more. The team never offered any hope. Gordon was a great listener and knows what really helps but the abuse in society has scared them straight into blindness. ps;, he was tested for drugs of other sorts and 2nd test came up false + .. a legitimate shame.
sure … but then again we are all human. As per my comment. they do have it hard.
Ps; if you have a half decent doc keep him her as long as you can … our family is still in midst of a absolute travesty and Etobicoke has few solid English speaking and well rounded docs. I had to go through the College website for hours on end to call 100+ GTA wide for me and family. god help us. Hold on to you doc if you like them 50%.
Heather Ross is an incredible cardiologist, but she is not a heart surgeon. It would have been nice if in copying the numerous US “Top Doctors” issues Toronto Life had paid more attention to editorial veracity.
This list is utterly incomplete without Shaf Keshavjee on it.
I too was at the Wasser for a couple of years. I found them MILDLY helpful, yet NOWHERE NEAR the comprehensiveness found in their Clinic – only on their Website!!! I waited continually7-8 months AFTER I was in the Clinic to get some Pain CBT/Mindfullness Programme they offer, but the evil Nurse Marilyn kept bumping me and bumping me with a new excuse each time. They try to sell you their Clinic, but my experience there was with a Doctor who was sooooooo grumpy and even mean! I never found proper pain management nor support from that Clinic. It’s a sham.
Pain CBT/Mindfullness Programme?? you got to be kidding me, i was in total dark as they never ever even after several months they were horrific. Yes marylin or whoever she was that meany bully was not nice. This place needs to be audited and spy cams brought in. Cut all and all funding immediately.
Dr. Flannery is a concerned, patient, understanding Doc. Knows how to drill down to the bottom of the problem pile and work upwards to regained mobility. It may take time, but he takes the time. Not many like him out there. Glad to see his name in the top Docs of Toronto – he deserves to be there.
What about the Doctors of chiropractic, dental medicine, veterinarian medicine, optometry??
Useful information shared.
Research has shown physical medicine treatments such as chiropractic that activate neurological reflexes stimulating the PAG and acupuncture which deactivates limbic system structures such as the amygdala provide significant pain relief for both nociceptive and neuropathic pain processes. This compared to the medical approach of spinal injections in which research shows that pain relief occurs in 50% of the patients with treatments needing to occur on a weekly basis results in a perceived bias of what the best type of pain medicine is. For those truly in pain physical medicine treatments such as manipulation and acupuncture along with exercise (dependent on heart rate) should always be tried prior to pharmacological intervention. If these treatments do not work, as every person is unique and their symptoms are unique, then pharmacological intervention and injections can be utilized. In addition, for patients it is your responsibility to take control of your health. If you have chronic pain, ensure that your doctor is qualified to evaluate and treat your pain. One simple way is to see if your doctor has obtained Diplomat status with the American or Canadian Academy of Pain Management. Credentialing is important, not only as it shows the doctor has taken the time to learn about the topic, but also in that a credentialed doctor is required to continue to learn about the topic which keeps them up to date on pain medicine research as medicine is every changing. As a Diplomat with the American and Canadian Academy of Pain Management I am required to take 100 hours of continuing education every 4 years in pain medicine. For more information on pain management please see my website. http://www.drmazzarella.com
Again, just saw this article pop up in my discus and it is a global travesty how poorly ratings and credit are given to those where no credit is due. Measure their success with hard facts and I plead to all rational and thinking people to speak to the real pain sufferers, real real patients who are the ones in need for real help.
With all due respect doc, from here on in any reference I make is strictly from an over educated / informed angle borderline Doctor perspective – and chiro was only a 2-3 day help. But it does and has saved endless lives and assisted many.
What about Dr. Essam Michael?? He is absolutely amazing and great at what he does! (ObGyn/Reproductive Endocrinologist).
Optometrists and chiropractors should not have Dr’s in front of their names.
Dr. Tirone David is the best surgeon I have ever encountered and I have had a few operations in my liftime. He saved my lift where other doctors didnt even know what they were looking at. I had an atrial myxoma which the Cardiologist I was seeing had only ever heard of it but had never seen a case. They flew Dr. David back to Toronto and operated on me within 2 days because as per his words “we gotta get this thing out quickly” because all it may have taken was me walking across a room and I could have died. He is a smart and great man with an awesome personality for a man with such success and I hope that he has the ability to help many more people in his career. Hope he doesn’t retire anytime soon.for the sake of others.
I had a dr. at Wasser but he was told to stop seeing his patients & see only new people. So I lost my pain dr. due to this new policy. Very poor.
Dr. David Lam http://ca.linkedin.com/pub/david-k-lam-md-dds-phd/64/b31/187 needs to be considered for the 2015 edition. I lost all sensation to my tongue from an injury and had severe burning pain. He operated on me, grafted a new nerve and restored all my feeling and taste! He is amazing.
I was a patient of Dr Sussman several years ago. While he successfully treated my hives, he did so without monitoring my liver and I ended up with damage to my liver. Simple routine blood work would have allowed him to adjust my dosage and not end up substituting one problem for another. Yes, he can treat allergies…but you end up another often more serious problem as a result
And who did the research on the Nephrologist? I’m sure he’s great…but the statement that St Mike’s is the only hospital in Canada doing incompatible transplants is simply false. I myself was in incompatible donor in 2009. The transplant was performed by Dr Robinette at Toronto General. I’m thrilled that other hospitals have picked it up, including St Mike’s, but they are NOT the only ones.
M waiting for hip replacement almost 1 year how long more it will take
Can anyone give me the direction I really don’t know m in pain almost 3 years
Yes but all that training( in one aspect of medical profession) is useless if you no good at the job. I was hospitalized with Pancolitis and the Dr. Anand the gi “specialist” (with 20 years experience)didn’t have a clue about my illness. He discharged me after one night leaving me untreated when a week earlier he treated me fir the exact same thing. Continue your hard work in medical studies, only to realize you are studying under the monopoly pharmaceutical system that has deluded the public for years.
Where is Dr. Jan Marak Gavel Top headache researcher is North America. Assistant head neurologist at the Univ. of Toronto, head plastic surgeon at Sunnybrook and top Sunnybrook neurologist, etc…etc…he reduced my cluster headaches and migraines from 90% of the time to nearly 0% with Varapamil, and an MRI and CT that had been so poorly read it was as if a kindergarden child drew them with crayons and wrote the results while on LSD. He was able to identify lesions from post concussion syndrome and found an acoustic neuroma the size of a walnut that the worthless radiologist described as “unremarkable”. He is outstanding. Another doctor that should be there is Dr. Jamarayan at St. Joeseph’s. A no-holds barred, no bull, doctor who has no issue taking on the professionalism of other doctors, and does not accept “business” as an excuse. “We’re ALL busy” he says. Others I know well are Dr. Joseph Mammaza at St. Michael’s, Dr. Ian Bookman at St. Joseph’s, EVERY doctor at Sick Kid’s Hospital, Dr. Benjamin Ogilvie-Harris, an incredible orthopaedic surgeon, Dr. Stephen Cartan, Humber Hospital, all the oncologists I had at Mount Sinai, and especially Dr. Kulwant Singh at Northeast Cancer Centre in Sudbury, not to mention Dr. Steven Sears, General Practitioner from Cobalt Ontario, the best doctor Temiskaming District Hospital, New Liskeard, Ontarto and Dr. Philip Smith at TDGH as well. Dr. Tirone David A magnificent skilled and compassionate man if there ever was one.
You missed two more for your list that I know of. Imagine having blood coming out your bum at 3 am, knowing your father had colon cancer in his 40s and you’re 59, going to local hospital Emerg at 4 am to find it packed with people waiting. Imagine how totally petrified you’d be, written all over your face. Imagine an angel of mercy triage doctor with beautifically handsome face and manner to match suddenly appearing at your side after only a very short time, putting his hands on your shoulders and saying he was going to look at you right away, but it probably isn’t bad or else you’d not be sitting there waiting to be seen. He examines you, says it’s not life threatening but because you’re so scared, he is going to arrange to fast track you to a colonoscopy by the best bum doctor in all of Canada. That was my experience in 2010 with multi-hospital night shift Emerg Ward specialist Dr. Karim Jessa, that night at North York General. The best bum doctor in Canada that Dr. Jessa got me in to be cared by turned out to be NYG Chief of Medicine and Program Director Dr. David Baron, same caring reassuring manner as Dr. Jessa, who did two complete all-the-way colonoscopies on me that several others years before had failed to accomplish, and said he removed 4 benign polyps, including 1 that he said was the largest he’d ever removed from anybody that was not cancerous. I finally started breathing again that day. If I were in any other country, I could not have afforded their superb care. Thank you CANADA ! Please add both those Doctors to your Best Doctors list.
please I need a doctor specialist in nerve and disc problems in nick and back, I want to come to Ontario at august for consultation and physiotherapy,please send the information to my email amnaabdulla28@gmail.com
My daughter has been a patient of dr sussman’s for almost a year and we don’t have any answers on her many allergies. We waited nearly 6 months for an appointment to get some test results and when we arrived there were still no results. The doctor shifted blame to the lab even though I had called to ask about her results multiple times and nobody seemed to notice that there weren’t any to be found. We had a second test done and were told we would get the results over the phone. This took over a month of calling almost every day and we still don’t have any useful information. Not to mention her biggest allergy wasn’t tested at all so we will have to go back for a third blood test! (Any of you taken a baby for a blood test? No fun)
Dr Sussman may be a good allergist but the mistakes that keep happening either by him or his support staff are rendering him useless to us and have made this process extremely stressful for us. We will be going elsewhere.